What is Contact Tracing?
Contact Tracing is also known as tracking. According to Wikipedia,
“In public health, contact tracing is the process of identification of persons who may have come into contact with an infected person (“contacts”) and subsequent collection of further information about these contacts. By tracing the contacts of infected individuals, testing them for infection, treating the infected and tracing their contacts in turn, public health aims to reduce infections in the population. Diseases for which contact tracing is commonly performed for include tuberculosis, vaccine-preventable infections like measles, sexually transmitted infections (including HIV), blood-borne infections, some serious bacterial infections, and novel infections (e.g. SARS-CoV and SARS-CoV-2). The goals of contact tracing are:
- To interrupt ongoing transmission and reduce spread of an infection
- To alert contacts to the possibility of infection and offer preventive counseling or prophylactic care
- To offer diagnosis, counseling and treatment to already infected individuals
- If the infection is treatable, to help prevent reinfection of the originally infected patient
- To learn about the epidemiology of a disease in a particular population”
Wikipedia, Contact Tracing, https://en.wikipedia.org/wiki/Contact_tracing Accessed 4/14/2020.
Contact Tracing is Nothing New as a Concept
Quarantine is an ancient practice. “The practice is first recorded in the Old Testament where several verses mandate isolation for those with leprosy. Ancient civilizations relied on isolating the sick, well before the actual microbial causes of disease were known.” Leslie S. Leighton, The History of Quarantines to Isolate The Sick Dates Back Thousands of Years, https://www.sciencealert.com/quarantines-have-been-used-to-try-keep-diseases-at-bay-for-thousands-of-years Accessed 4/14/2020.
Quarantine was just one of the methods used in the early 20th century during the 1918 Spanish Flu pandemic that are still in use today. “They had the kind of social distancing measures that we’re still using today: isolation, quarantine, masks, hand-washing, staggering rush hour so you don’t have massive crowds in the metro and the streets. Those are techniques that are very ancient. People have always understood you have to keep the healthy and the sick separate,” said pandemic history Pale Rider author Laura Spinney. https://www.vox.com/2020/3/9/21164957/covid-19-spanish-flu-mortality-rate-death-rat
that are still in use today. “They had the kind of social distancing measures that we’re still using today: isolation, quarantine, masks, hand-washing, staggering rush hour so you don’t have massive crowds in the metro and the streets. Those are techniques that are very ancient. People have always understood you have to keep the healthy and the sick separate,” said pandemic history Pale Rider author Laura Spinney. https://www.vox.com/2020/3/9/21164957/covid-19-spanish-flu-mortality-rate-death-rat
Two basic tools of communicable disease control in modern times have been quarantine and contact tracing. “The eradication of smallpox, for example, was achieved not by universal immunization, but by exhaustive contact tracing to find all infected persons.[1] This was followed by isolation of infected individuals and immunization of the surrounding community and contacts at-risk of contracting smallpox.” Wikipedia, ibid.
Here is a chart explaining Contact Tracing: 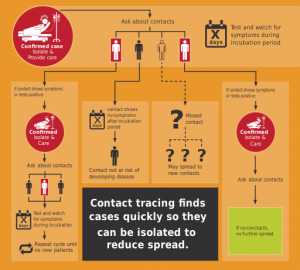 ” General illustration of Contact Tracing based off of CDC-material, By CFCF – Own work, CC BY-SA 4.0, https://commons.wikimedia.org/w/index.php?curid=88348237
” General illustration of Contact Tracing based off of CDC-material, By CFCF – Own work, CC BY-SA 4.0, https://commons.wikimedia.org/w/index.php?curid=88348237
CFCF / CC BY-SA (https://creativecommons.org/licenses/by-sa/4.0) found on Wikipedia at https://commons.wikimedia.org/wiki/File:Contact-tracing_adapted.svg Accessed on 4/14/2020
Covid-19 Contact Tracing is different
Is all contact tracing the same? No–but how and why? First, Covid-19 is different. The Centers for Disease Control and Prevention (CDC) has identified our current problem virus as one of seven viruses that have been detected since the 1960s. It explains it thusly:
Human Coronavirus Types
Coronaviruses are named for the crown-like spikes on their surface. There are four main sub-groupings of coronaviruses, known as alpha, beta, gamma, and delta.
Human coronaviruses were first identified in the mid-1960s. The seven coronaviruses that can infect people are:
Common human coronaviruses
- 229E (alpha coronavirus)
- NL63 (alpha coronavirus)
- OC43 (beta coronavirus)
- HKU1 (beta coronavirus)
Other human coronaviruses
- MERS-CoV (the beta coronavirus that causes Middle East Respiratory Syndrome, or MERS)
- SARS-CoV (the beta coronavirus that causes severe acute respiratory syndrome, or SARS)
- SARS-CoV-2 (the novel coronavirus that causes coronavirus disease 2019, or COVID-19)
People around the world commonly get infected with human coronaviruses 229E, NL63, OC43, and HKU1.
Sometimes coronaviruses that infect animals can evolve and make people sick and become a new human coronavirus. Three recent examples of this are 2019-nCoV, SARS-CoV, and MERS-CoV.
Page last reviewed: February 15, 2020. Content source: National Center for Immunization and Respiratory Diseases 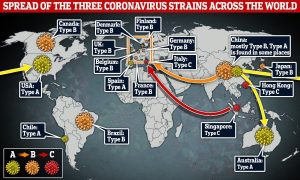
(NCIRD), Division of Viral Diseases” https://www.cdc.gov/coronavirus/types.html Accessed 4/15/2020.
The present Covid-19 has mutated into a number of strains. This graphic shows the distribution of just three.
Tracking, Vaccines, and Testing
Derek Thompson, Staff Writer at The Atlantic, wrote in early April that contact tracing could free United States residents from having to quarantine. https://www.theatlantic.com/ideas/archive/2020/04/contact-tracing-could-free-america-from-its-quarantine-nightmare/609577/ In “The Technology That Could Free America From Quarantine” he writes: “Contact tracing is working in South Korea and Singapore. But it raises privacy issues.”
According to Jonathan Ellen in his article “Tracking Infection”, contact tracing will be essential to controlling Covid-19 when testing is fully implemented. Jonathan M. Ellen, March 30, 2020 Covid-19 Health Care https://www.city-journal.org/covid-19-contact-tracing
Dr. Ellen explains, “The most effective means of interrupting transmission, of course, is to develop and deploy a vaccine that, by providing high levels of immunity, prevents an uninfected person from acquiring the virus from an infected person. By blocking transmission, vaccines not only prevent infection and complications; they also prevent one person from infecting many others. Unfortunately, we are at least a year away from having a vaccine for Covid-19.
“But public-health departments do have tools for battling infectious diseases for which there is no vaccine. Contact tracing, for example, is a focused strategy for breaking transmission chains and controlling the spread of disease. It involves identifying infected persons; taking steps to prevent an infected person from further spreading infection, whether through isolation or treatment, if an effective treatment option exists; identifying those with whom the infected person may have been in close contact while infectious; and, finally, locating and testing these close contacts. If a close contact is found to be infected, the disease-investigation process starts again. The Centers for Disease Control’s Ebola control strategy illustrates how contact tracing can work.
“Adapting this process to Covid-19, it’s important to identify asymptomatic or mild cases as well as severe cases because these cases can transmit the virus, too. In addition, we need to apply the CDC’s definition of a “close contact” to Covid-19. Being within six feet of someone for a prolonged period; or caring for, visiting, or living with a Covid-19 infected person, qualifies as close contact. South Korea worked from this definition, and it has been credited with reducing the proliferation of cases there. South Korea’s success so far, Science reports, owes to “the most expansive and well-organized testing program in the world, combined with extensive efforts to isolate infected people and trace and quarantine their contacts.”
“To work effectively, though, contact tracing depends on certain preconditions—especially no existing barriers to testing. As long as testing remains incomplete or uncertain, public-health officials cannot draw lines of transmission accurately. The disease burden—its penetrance into the community—also must be low enough that it is practical for public-health officials to investigate people identified as infected, whether symptomatic or not; and the disease must not be so widespread that the chains of transmission become blurred or the area’s hospital system already overwhelmed with cases.
“Even after infection has peaked and hotspots cool down, there will likely continue to be sporadic new cases. Contact tracing is most effective as a means of containing flareups. Applying this strategy in low-prevalence communities can prevent exponential growth in new cases, save lives, and protect health-care systems and their frontline workers.”
Jonathan Ellen, M.D., is a pediatrician, an epidemiologist, public health academician, and the former CEO of Johns Hopkins All Children’s Hospital.
In Virginia, a new Covid-19 contact tracing App has been launched. 
However, in other places of high community spread, health officials are slowing their contact tracing efforts, according to a recent New York Times article. https://www.nytimes.com/live/2020/11/24/world/covid-19-coronavirus/officials-scale-back-contact-tracing-efforts-in-the-us-saying-they-cannot-keep-up The article also quoted Crystal Watson, an assistant professor at Johns Hopkins Bloomberg School of Public Health, as saying “It still saves lives, it still breaks chains of transmission. Every person we can get to quarantine at home, who is not out in the community — that contributes to reduction in incidence.”